
Table of Contents
- Why Parents Search for a Child Autism Checklist
- What Is a Child Autism Checklist and How Should It Be Used?
- Child Autism Checklist by Age and Developmental Stage
- Social Communication and Interaction Signs to Look For
- Behavioural and Sensory Signs on a Child Autism Checklist
- Common Autism Screening Tools Parents May Encounter
- When a Checklist Suggests the Need for an Autism Assessment
- What Happens After an Autism Diagnosis
- FAQs
- Conclusion
In Focus: Child Autism Checklist Summary
- This guide is for parents of babies, toddlers, and young children who have concerns about autistic traits or developmental differences.
- Autism signs commonly involve social situations, sensory processing differences, and repetitive or restricted behaviours.
- Presentation can vary significantly by age, developmental stage, and gender.
- Screening checklists are not diagnostic tools and cannot confirm or rule out autism.
- A full autism assessment can be considered when multiple signs are present across various settings and impact daily life or learning.
Why Parents Search for a Child Autism Checklist
Most parents look for autism checklists during their quiet times, when concerns are not pressing. You may see differences in your child’s communication, play, or behaviours and ask if these are the result of a developing individual personality, varying levels of development, or a potential concern that warrants further attention. A checklist for many families helps them to document their own observations and decrease their anxiety when uncertainty is apparent.
It is important to be clear, however, about what a child autism checklist can and cannot do. Checklists are screening tools, not diagnostic instruments. They are designed to highlight patterns over time, not isolated behaviours or single moments.
AuDHD Psychiatry is a UK-based neurodevelopmental assessment and diagnosis centre specialising in autism and ADHD across the lifespan. We regularly support families who arrive with a sense that “something doesn’t quite fit”. Used thoughtfully, a checklist can be a valuable bridge between parental intuition and professional assessment.
If concerns persist, a professional autism assessment can offer clarity, understanding, and appropriate support for your child’s needs.

What Is a Child Autism Checklist and How Should It Be Used?
A child autism checklist is a methodical enumeration of behaviours and developmental characteristics linked to autism spectrum disorders. These instruments are utilised by parents, caregivers, or specialists to document the persistence and regularity of specific traits over a certain period.
What a Checklist Measures
Most child autism checklists focus on four core areas:
- Social communication – how a child uses and understands language, gestures, facial expressions, and back-and-forth interaction
- Social interaction – interest in others, shared attention, peer relationships, and social reciprocity
- Repetitive behaviours and restricted interests – repetitive movements, rigid routines, or intense focus on specific topics
- Sensory processing differences – heightened or reduced responses to sounds, textures, movement, taste, or visual input
Although these areas are aligned with respected diagnostic models applicable in formal evaluations, checklists identify only preliminary clinical signs and not the underlying clinical intricacies.
What a Checklist Cannot Do
A child autism checklist cannot:
- Confirm a diagnosis of autism
- Exclude autism if scores appear low
- Differentiate autism from other developmental or mental health conditions
- Replace comprehensive diagnostic assessments carried out by trained clinicians
It’s important to note these limitations. Children may score below thresholds and still be autistic, particularly if they mask traits, have high verbal ability, or are female. Conversely, some children may show autistic-like behaviours related to anxiety, language delay, trauma, or sensory processing difficulties without meeting diagnostic criteria.
Why Checklists Are Still Useful for Parents
Though checklists for child autism have limitations, with care and consideration, they can be quite useful. They assist parents in structuring thoughts about their child’s behaviour and differences in development, as opposed to thinking in fragmented memories or comparing with other kids. This can provide clarity in discussions with healthcare professionals, teachers or health visitors, especially when concerns have been there for a long time.
Checklists can assist in pattern tracking over a duration of time to see if differences are consistent, growing, or just situational. Most importantly, they can help answer whether it makes sense to look for additional support or referrals.

Child Autism Checklist by Age and Developmental Stage
Autism may look different at every age. Developmental expectations change rapidly in early childhood, and autistic traits may become more or less noticeable depending on environmental demands.
Babies and Toddlers (6–24 Months of Age)
In infants and toddlers, autism-related differences often involve early social communication and sensory responses rather than clear behavioural patterns.
Parents may notice:
- Limited or inconsistent eye contact during interaction
- Reduced response to name despite normal hearing
- Fewer shared smiles, facial expressions, or attempts to engage others
- Differences in joint attention, such as limited pointing or showing objects
- Unusual reactions to sound, touch, or movement
- Delays or differences in babbling, gestures, or early words
At this stage, it is essential to consider overall developmental milestones rather than isolated traits. Some children show early signs that later lessen, while others become more apparent with age.
Young Children (2–5 Years of Age)
During the preschool years, social and communication differences often become clearer as peer interaction and imaginative play develop.
Checklist items may include:
- Delayed speech or unusual language patterns
- Limited pretend play or repetitive play themes
- Repetitive movements i.e. hand flapping or rocking
- Distress around changes in routine or transitions
- Difficulty engaging in reciprocal play with peers
- Strong sensory preferences or aversions
Some autistic children at this age may have extensive vocabularies, but have difficulty with the mechanics of conversation, integrating appropriate social cues, and the rhythms of social engagement.
Primary School-Age Children (5–11 Years of Age)
Some autistic children at this age may have extensive vocabularies, but have difficulty with the mechanics of conversation, integrating appropriate social cues, and the rhythms of social engagement.
Parents and teachers may observe:
- Ongoing difficulties with social skills and peer relationships
- Literal interpretation of language and difficulty understanding social rules
- Heightened anxiety or emotional regulation challenges
- Restricted interests that dominate conversation or play
- Masking behaviours at school followed by emotional exhaustion at home
If you are noticing these patterns, our detailed guide: Child Autism Signs explores age-specific presentations in more depth.

Social Communication and Interaction Signs to Look For
Differences in social communication and social interaction are central to autism, but they can present very differently from one child to another. These differences are best understood as qualitative variations in how a child communicates and relates to others, rather than simple delays or deficits. A child autism checklist often focuses on how consistently these patterns appear across time and situations.
Social Communication Differences
A child autism checklist may highlight:
- Limited back-and-forth conversation
- One-sided communication focused on specific interests
- Literal understanding of language, jokes, or sarcasm
- Difficulty using or interpreting gestures and facial expressions
- Reduced ability to adapt communication to different social contexts
The patterns outlined should not be interpreted as disinterest in people or relationships. Children on the autism spectrum often wish to engage with others socially, but may do so with atypical processing of language and other forms of communication. Studies indicate that language processing, alongside other forms of communication, not being in synch with others, can be viewed as an alternative way of communicating, and not as evidence of a lack of understanding socially. This is particularly true of children who have good verbal communication, but have difficulty with the so-called social rules of a conversation.
Social Interaction in Everyday Settings
The challenges children face when interacting socially can vary, depending on the context. This includes the following:
- At home: preference for solitary play or engaging with others when it is on their terms
- At school or nursery: difficulty being a part of group activities or having an understanding of the relationships between individual members of the group
- Across all contexts: presentation varies depending on the organisation of the environment and the existing sensory demands.
Having consistency in behaviour across a variety of contexts provides more important information than having behaviour in only one context. For example, a child may display socially appropriate behaviour in a school context, but if that child is emotionally drained when they get home, they may be hiding their social challenges.
Behavioural and Sensory Signs on a Child Autism Checklist
Features on a child autism checklist that can cause parental concern are the differences in sensory processing and the behavioural style shown. These features are not negative in any way. They can be signalled from the behavioural style and sensory processing differences when a child is exhausted and overwhelmed in the most environmentally demanding of situations. The features mentioned will be problematic in the most environmentally demanding situations and will be consistent across various situations rather than being occasional.
Repetitive Behaviours and Movements
Here are some examples:
- Hand flapping, spinning, pacing, and other similar movements
- Looking at parts of an object, focusing on parts of objects, or repetitive play.
- Distress when routines are disrupted
- Unyielding, strong expectations about how tasks should be accomplished.
Such behaviours are often self-soothing and help the child cope with anxiety, sensory overload, or even help them feel in control of their environment. These behaviours are often mischaracterised as purposeless or aimless when, in fact, they are occupationally and clinically recommended and adapt to stimuli in their environment to make it less overwhelming or unpredictable. Concern for these behaviours arises when they are sufficiently present to disrupt learning, daily tasks, or family engagement.

Sensory Processing Differences
Children with autism may experience the following challenges:
- Out-of-control reactions to busy places and loud noises
- Clothing textures, the texture of foods, and the smell of foods
- The need to be moved, pressured, or stimulated visually.
Children present with varying degrees of sensory intolerance, depending on the context, stress level, and fatigue. Without question, the pronounced sensory challenges of children with autism, occupational therapy, and sensory integration are invaluable in assisting with sensory regulation, daily functioning, and structures at home or school.
The Role of Teachers, GPs, and Other Professionals
While parent observations are central to any child autism checklist, input from professionals can add important context. Teachers, early years staff, and childcare providers observe children in structured, socially demanding environments where autistic differences may be more apparent. They may notice patterns such as difficulties with group work, social rules, emotional regulation, or sensory overwhelm that are less visible at home.
A child’s doctor, GP, or health visitor may also contribute by ruling out hearing, speech, or other developmental concerns and supporting referrals when appropriate. NICE guidance emphasises the importance of gathering information from multiple settings and informants, rather than relying on a single viewpoint. When parental concerns align with observations from school or healthcare professionals, this often strengthens the case for further assessment and ensures a more balanced understanding of the child’s needs.
Common Autism Screening Tools Parents May Encounter
While researching autism, parents may encounter screening tools that differ in format, age, and purpose. These tools do not provide diagnoses, but rather provide insight into whether further evaluations may be necessary.
Parent-Completed Screening Tools
Common examples include:
- Modified Checklist for Autism in Toddlers (M-CHAT) – commonly used with toddlers and younger children
- Childhood Autism Spectrum Test (CAST) – more often encountered for primary school-aged children
These tools are based on parent observations and provide a total score on whether further assessments are warranted. These tools do not verify or rule out an autism diagnosis, and should not be treated in isolation. Some parents may appreciate starting their autism screening with a free online autism screener for children.
Clinician-Led Screening and Assessment Instruments
Healthcare professionals may use:
- Childhood Autism Rating Scale (CARS)
- A sampled structured developmental history from parents
- Direct observations of the child
- Input from school, daycare, and family
These elements are not stand-alone tests. Instead, they are used in the context of a larger diagnostic assessment.
Understanding Scores and Results
A higher score suggests an increased likelihood of autistic traits but does not equal a diagnosis. Factors such as masking, gender differences, and co-occurring conditions affect results. Interpretation by trained healthcare professionals is essential.
When a Checklist Suggests the Need for an Autism Assessment
The most useful checklists show patterns of a child’s behavior as opposed to isolated behaviours. It’s true that singular behaviours do not confirm autism. However, behaviours that are persistent or combinations of behaviours may warrant a more formal assessment. We do not want to label the child, but simply to understand the developmental profile to see if more support is needed.
Signs That Warrant Further Evaluation
Consider seeking assessment when:
Multiple signs appear across environments
Both home and other places, like nursery and school, show differences. If the differences are consistent across all environments, then there are likely some underlying neurodevelopmental differences rather than situational ones.
Differences impact learning, relationships, or emotional well-being
This may include difficulties accessing the curriculum, increased anxiety, frequent emotional overwhelm, or challenges forming and maintaining peer relationships.
Concerns are shared by teachers, health visitors, or other professionals
When professionals independently raise similar observations, this can strengthen the case for further evaluation and support referral pathways.
Traits persist over time rather than resolving
Many children show temporary developmental variations. Ongoing traits that remain consistent or become more pronounced as social demands increase are often more clinically relevant.
If you would like to explore assessment pathways or costs, you may find our guide to the cost of a private autism assessment helpful: Private Autism Assessment Cost.
Who Can Assess a Child for Autism in the UK
Autism assessments may be conducted by:
- Developmental paediatricians (UK spelling retained)
- Clinical psychologists or psychiatrists
- Multidisciplinary diagnostic services
Private assessments can reduce waiting times and provide detailed, individualised reports.
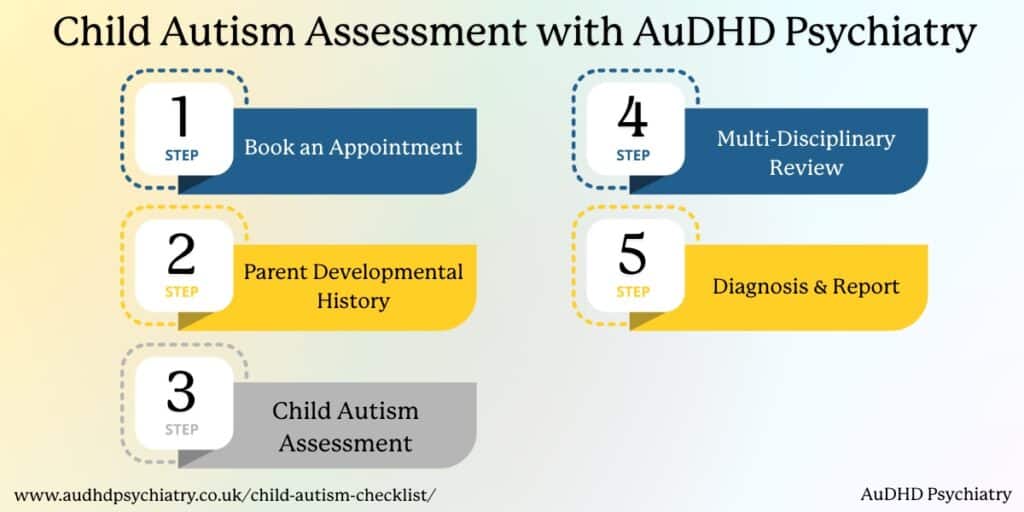
AuDHD Psychiatry’s Child Autism Assessment
You are welcome to book directly with AuDHD Psychiatry. Our child autism assessment process is designed to be clear, supportive, and developmentally appropriate, while remaining clinically robust and aligned with UK best practice.
Step 1 – Book an Appointment
Appointments can be booked at a time that works for your family, with no GP referral required. An initial screening conversation helps us understand your concerns, including early developmental differences, school feedback, and any questions around masking or behaviour across settings.
Step 2 – Parent Developmental History
A detailed developmental history is gathered through a structured discussion with an experienced clinician. This covers early childhood development, communication, social interaction, sensory differences, strengths, and challenges at home and in education.
Step 3 – Child Autism Assessment
Your child takes part in a structured, child-appropriate autism assessment. This is informed by gold-standard approaches and focuses on observing natural communication, interaction, and behaviour in a supportive, low-pressure environment.
Step 4 – Multi-Disciplinary Review
Information from the parent history, child assessment, and any available school or professional reports is reviewed by clinicians as part of a multidisciplinary process, in line with NICE guidance.
Step 5 – Diagnosis & Report
You receive a clear outcome, a comprehensive written report, and a feedback appointment to discuss findings and practical next steps for support at home and school.
Why Does Early Identification and Diagnosis Matter?
Research studies suggest that autism profiles can change across childhood, with some children showing reduced support needs over time and others experiencing increased challenges. Early identification supports access to early intervention, educational adjustments, and mental health support, reducing long-term strain for autistic children and their families.
What Happens After a Child Gets Diagnosed for Autism
Understanding Your Child’s Profile
A diagnosis focuses on understanding strengths, differences, and support needs rather than assigning a label alone. This may include discussion of autism levels and functional impact, such as Level 2 autism, where an autistic child often requires substantial support across multiple settings.
Post-Diagnostic Support Options
Following diagnosis, support may involve a combination of:
- Speech and language therapy to support communication and interaction
- Occupational therapy to address sensory regulation and daily living skills
- Educational planning, including special educational needs (SEN) support and reasonable adjustments at school
Supporting the Whole Family
Post-diagnostic guidance often extends beyond the child. Parents and carers may receive practical advice, support with school liaison, and signposting to autism support networks. This broader approach can reduce uncertainty and help families feel more confident advocating for their child’s needs.
Frequently Asked Questions About Child Autism Checklists
Can a child pass a checklist and still be autistic?
Yes. Many autistic children score below thresholds, particularly girls or those who mask traits.
Do autism signs change as children grow older?
They can. Research indicates that autism presentation may increase, decrease, or remain stable across childhood.
Are online autism checklists reliable?
They can be helpful screening tools, but should never replace professional assessment.
Can girls score lower on autism checklists?
Yes. Girls often present differently and may mask autistic traits more effectively. Our Female Autism Checklist and guide to Autism Symptoms in Girls explore this in more detail.
Should I wait or seek assessment now?
If concerns persist and impact daily life, seeking assessment is usually preferable to waiting. We understand that you may have questions you’d like answered before deciding, so we’ve made sure to have our clinicians or trained specialists ready to help. Contact us for a child autism screening call if you’d like recommendations on whether or not an autism diagnostic pathway should be considered.
Child Autism Checklist: Conclusion
A child autism checklist can be a valuable starting point for understanding your child’s development, but it is not a diagnosis. Its greatest value lies in helping parents notice patterns, organise concerns, and seek appropriate professional guidance.
Trust your observations. If something feels significant or persistent, it deserves attention. Timely assessment can provide clarity, reassurance, and access to tailored support that benefits both your child and your family.
If you are considering next steps, book a call with us today for a comprehensive, neurodivergent-affirming autism assessment designed to support understanding rather than judgment.
References
- Hus, Y., & Segal, O. (2021). Challenges surrounding the diagnosis of autism in children. Neuropsychiatric Disease and Treatment, Volume 17, 3509–3529. https://doi.org/10.2147/ndt.s282569
- De L Martínez-Pedraza, F., & Carter, A. S. (2009). Autism spectrum disorders in young children. Child and Adolescent Psychiatric Clinics of North America, 18(3), 645–663. https://doi.org/10.1016/j.chc.2009.02.002
- Johnson, C. P., & Myers, S. M. (2007). Identification and evaluation of children with autism spectrum disorders. PEDIATRICS, 120(5), 1183–1215. https://doi.org/10.1542/peds.2007-2361
- Maestro, S., Muratori, F., Cesari, A., Cavallaro, M., Paziente, A., Pecini, C., Grassi, C., Manfredi, A., & Sommario, C. (2005). Course of autism signs in the first year of life. Psychopathology, 38(1), 26–31. https://doi.org/10.1159/000083967
- Ozonoff, S., Iosif, A., Baguio, F., Cook, I. C., Hill, M. M., Hutman, T., Rogers, S. J., Rozga, A., Sangha, S., Sigman, M., Steinfeld, M. B., & Young, G. S. (2010). A prospective study of the emergence of early behavioral signs of autism. Journal of the American Academy of Child & Adolescent Psychiatry, 49(3), 256-266.e2. https://doi.org/10.1016/j.jaac.2009.11.009
You Might Also Like
Contact Us
We’re here to answer any questions you might have.
Get in Touch
Opening Hours
Contact Form
We’re here to help. Reach out and we’ll get back to you within 24 hours (Monday – Friday).



Leave a Reply