Table of Contents
- What Is ADHD?
- Why ADHD Increases the Risk of Addiction
- The Neurobiology of ADHD and Addiction
- Types of Addiction Associated with ADHD
- Managing ADHD and Addiction
- Breaking the Cycle: When to Seek Help
- FAQs
- Conclusion
In Focus:
- People with ADHD are two to three times more likely to develop a substance use disorder than those without ADHD.
- The same neurobiological differences that drive ADHD symptoms, particularly around dopamine, also increase vulnerability to addictive behaviours.
- Both substance addictions and behavioural addictions are more common in people with ADHD.
- Untreated ADHD significantly raises addiction risk; appropriate treatment can meaningfully reduce it.
- Effective support for co-occurring ADHD and addiction requires addressing both conditions simultaneously.
The relationship between ADHD and addiction is one of the most consistently documented findings in neurodevelopmental research. People with attention deficit hyperactivity disorder (ADHD) are significantly more likely to develop substance use disorders, engage in compulsive behaviours, and struggle with addiction across their lifetimes compared to the general population.
This is not a coincidence. The neurological differences that characterise ADHD, particularly those affecting dopamine regulation, impulse control, and the brain’s reward system, overlap substantially with the mechanisms that drive addictive behaviour. Understanding this connection is essential, both for individuals affected and for the professionals supporting them.
If you recognise these patterns in yourself or someone close to you, understanding the why behind them is often the first step towards meaningful change. Take our free adult ADHD self-test; it takes just a few minutes and could be a useful first step. No referral needed.
Understanding ADHD
Attention deficit hyperactivity disorder (ADHD) is a neurological disorder that affects how the brain regulates attention, activity, and impulse control. It is one of the most common mental health conditions in both children and adults, though it remains significantly underdiagnosed, particularly in women and those who present without obvious hyperactivity.
ADHD and addiction statistics tell a striking story. Research consistently shows that adults with the condition are two to three times more likely to develop alcohol use disorder, and rates of drug addiction, nicotine dependence, and behavioural addictions are all elevated compared to those without a diagnosis. Childhood ADHD, in particular, is a strong predictor of substance use problems in early adulthood, especially when ADHD goes undiagnosed or unsupported.
How ADHD Presents in Life
ADHD symptoms are divided into three presentations: predominantly inattentive, predominantly hyperactive-impulsive, and combined. Most adults present with a combination of both.
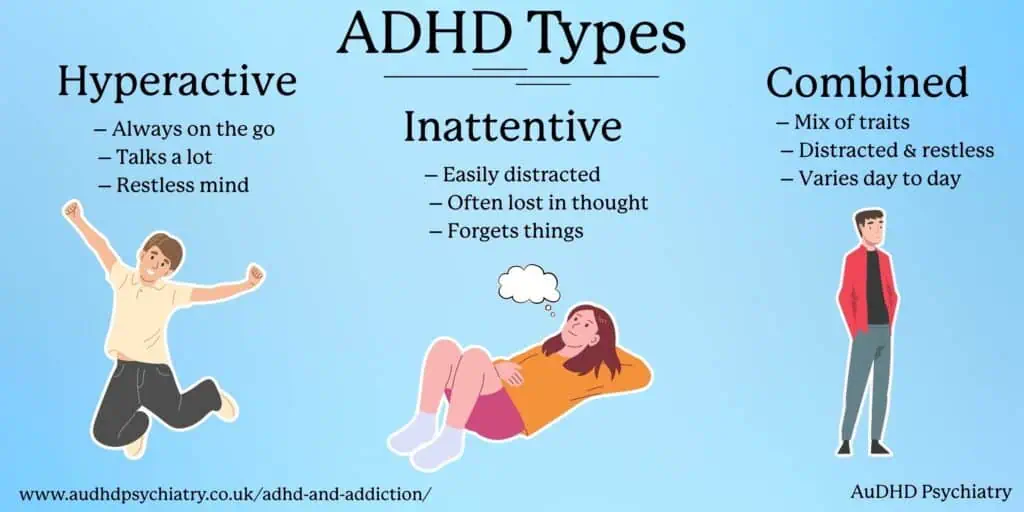
Inattention symptoms include:
- Difficulty sustaining attention on tasks that require prolonged mental effort
- Frequently losing items, missing deadlines, or forgetting appointments
- Poor organisation and difficulty managing time effectively
- Being easily distracted by external stimuli or internal thoughts
- Difficulty completing tasks once the initial interest fades
Hyperactivity-impulsivity symptoms include:
- Acting without thinking through consequences; impulsive behaviour
- Difficulty waiting, interrupting others, or needing constant stimulation
- Restlessness, fidgeting, or an internal sense of being “on the go”
- Talking excessively or blurting out responses before questions are finished
Emotional dysregulation, the difficulty managing intense emotions, tolerating frustration, and recovering from setbacks, is now widely recognised as a core feature of ADHD, even if it does not appear in formal diagnostic criteria. You can read more in our article on ADHD and emotional dysregulation.
ADHD Across the Lifespan
ADHD does not disappear in adulthood, though its presentation can shift. Hyperactivity often becomes internalised; impulsive behaviour may become more subtle but no less costly. Adult ADHD is associated with higher rates of relationship difficulties, employment instability, and mental health challenges—and addiction risk remains elevated throughout.
For young people, the teenage years and early adulthood represent a particularly vulnerable window. This is when alcohol and drug use typically begins, and when undiagnosed ADHD in adolescents creates conditions where risky activities and substance misuse can take hold with little resistance.
Why ADHD Increases the Risk of Addiction
Dopamine Deficiency and Reward Dysregulation
ADHD is fundamentally a disorder of dopamine regulation. The brains of people with ADHD have reduced dopamine activity, particularly in the circuits that govern reward, motivation, and sustained effort. This means that everyday activities often fail to generate sufficient reward signals — leaving people seeking external sources of stimulation to feel engaged or satisfied. You can read more about this in our guide to how ADHD affects the brain.
Addictive substances and behaviours, whether alcohol, nicotine, gambling, or social media, all produce rapid, intense surges of dopamine. For the ADHD brain, which is chronically under-stimulated, these effects feel disproportionately rewarding. The drive toward immediate reward over delayed gratification is not a character flaw; it is a neurological reality.
ADHD-Related Impulsivity
Impulsivity is one of the most direct pathways between ADHD and addiction. Acting without fully considering consequences, difficulty stopping once started, and a reduced ability to tolerate frustration all contribute to patterns of addictive behaviour. This is particularly relevant during the teenage years, when social pressure around substance use is highest and prefrontal development is still ongoing.
Self-Medication and Coping Strategies
Many people with undiagnosed ADHD discover (often unconsciously) that certain substances temporarily quiet the noise. Alcohol may reduce restlessness; nicotine or caffeine may improve focus; cannabis may ease anxiety. These are common ADHD symptoms that many people attempt to manage themselves, long before receiving any formal support. The problem is that this self-medication often leads to substance dependence, and the relief it offers becomes shorter-lived as tolerance builds.

ADHD and Co-Occurring Mental Health Conditions
ADHD rarely travels alone. Anxiety disorders, depression, and trauma-related conditions all co-occur with ADHD at elevated rates, and each adds its own layer of risk when it comes to addiction. Low self-esteem, frequently a consequence of years of struggling with unmanaged ADHD symptoms, is itself a significant contributor to substance use problems.
People managing multiple conditions often find that alcohol or drugs offer the fastest available relief from mental distress. Without proper diagnosis and support, these patterns can become deeply entrenched.
If you’ve reached this point and have been wondering whether ADHD might be at the root of some of your difficulties? Take our free adult ADHD self-test; it’s quick, confidential, and a helpful first step to determining whether a full assessment may help.
The Neurobiology of Addiction and ADHD
Understanding why ADHD and addiction so often co-occur requires a brief look at what both conditions share at the neurobiological level.
Addiction researchers describe the addiction cycle in three stages:
- Binge and intoxication
- Withdrawal and negative affect, and
- Preoccupation and anticipation.
At each stage, the brain’s dopamine and stress systems interact in ways that reinforce continued use despite negative consequences. In people with ADHD, these systems are already dysregulated before any substance enters the picture.
The mesolimbic dopamine system, the brain’s primary reward circuit, shows reduced activity in ADHD, making naturally rewarding experiences feel insufficient. Addictive substances and behaviours target this exact system, flooding it with dopamine and producing effects that feel uniquely powerful for the ADHD brain. At the same time, impaired executive control in the mesocortical system means that the brakes—the ability to pause, reflect, and choose differently—are less effective. The result is a brain that is simultaneously more attracted to addictive rewards and less equipped to resist them.
Types of Addiction Associated with ADHD
Substance Addictions
Alcohol addiction and alcohol use disorder are among the most commonly documented co-occurring conditions in this neurodevelopmental profile. ADHD and drug addiction, including cannabis use disorders, stimulant misuse, and opiate dependence, are also significantly more prevalent. Nicotine and vaping addiction are particularly common in young people with ADHD, with some research suggesting rates two to three times higher than in the general population.
The relationship between ADHD and substance abuse is also worth noting. Prescription stimulants such as methylphenidate and amphetamines are first-line treatments for ADHD and, when taken as prescribed, actually reduce rather than increase addiction risk. However, recreational use of stimulants, or taking higher doses than prescribed, can be problematic, particularly in those without a formal diagnosis.
Sedatives, tranquilisers, and illegal drugs such as opiates and hallucinogens are also used at higher rates in people with ADHD, often as attempts to manage overstimulation, anxiety, or the relentless mental activity that characterises the condition.

Behavioural Addictions
Behavioural addictions are often overlooked in discussions of ADHD, but the connection is just as neurologically grounded. Internet addiction, gaming addiction, gambling, shopping addiction, and sexual or pornography addiction all activate the brain’s reward system in ways that are particularly compelling for people with ADHD.
Social media addiction deserves special mention. The constant stimulation, immediate reward, and unpredictable notification patterns of social media platforms are almost tailor-made for the ADHD reward system. Screen time and social media use have become significant areas of concern in adolescents and young adults with ADHD, where addictive engagement can displace sleep, relationships, and daily functioning.
Food addiction, love and relationship addiction, and other reward-based compulsive behaviours also appear more frequently in people with ADHD. The common thread in all of these is instant gratification—the ability to produce a rapid dopamine hit in a brain that is chronically under-rewarded by ordinary life.
Managing ADHD and Addiction
ADHD Medication and Addiction Risk
One of the most persistent concerns people raise is whether ADHD medication might itself be addictive. The evidence is reassuring: when taken as prescribed under proper medical supervision, stimulant medications do not carry a meaningful addiction risk for people with ADHD. In fact, multiple studies show that appropriate stimulant treatment in childhood and adolescence is associated with a lower risk of subsequent substance use disorders, not a higher one.
For those where stimulant medications are not appropriate, non-stimulant medications such as atomoxetine offer an evidence-based alternative with no misuse potential. Any medication decisions should always be made collaboratively with a qualified clinician.
Why Quitting Addiction Can Be Harder with ADHD
People with ADHD often find addiction recovery more challenging than those without the condition. This is partly because the same impulsivity and reward-seeking that drove the addiction make sustained behaviour change more difficult. But it is also because, without treatment for the underlying ADHD, the drive to self-medicate remains, and another addictive pattern may emerge in place of the one being addressed.
Integrated Treatment Approaches
The most effective treatment for co-occurring ADHD and addiction addresses both conditions simultaneously rather than sequentially. Dual diagnosis treatment programmes, those specifically designed for mental health conditions alongside substance use disorder, produce substantially better outcomes than programmes that treat only the addiction.
Cognitive behavioural therapy (CBT) is the best-evidenced psychological approach for both conditions. It helps people identify the thinking patterns and behaviours that maintain both ADHD difficulties and addictive cycles, and builds practical skills for managing them. Alongside CBT, ADHD-specific support, support groups, and structured treatment plans tailored to the individual’s needs all play an important role.

Breaking the Cycle: When to Seek Help
If you recognise the patterns described in this article, whether in yourself or someone close to you, seeking professional help is worth it, and it does not have to start with a major commitment.
A good first step is exploring whether ADHD may be a contributing factor. Many people who have lived with untreated ADHD for years find that an accurate diagnosis changes everything. It reframes the struggle, informs the treatment plan, and often reduces the drive to self-medicate. If you haven’t yet been assessed, you can book a comprehensive ADHD assessment with our team directly.
If addiction is already a concern, please speak to your GP or a specialist service. Withdrawal from alcohol, benzodiazepines, or opiates can be medically serious and should not be attempted without professional guidance. The combination of ADHD support and addiction treatment, delivered together, offers the best chance of lasting recovery.
Frequently Asked Questions
Does ADHD cause addiction?
ADHD does not directly cause addiction, but it significantly raises the risk. The neurobiological overlap between ADHD and addiction, particularly around dopamine regulation and impulse control, means that people with ADHD are substantially more vulnerable to developing substance use disorders and behavioural addictions.
Is addiction more common in people with ADHD?
Yes. Research consistently shows that people with ADHD are two to three times more likely to develop alcohol use disorder, and rates of drug abuse, nicotine dependence, and behavioural addiction are also significantly elevated. The risk is particularly high in those with untreated or undiagnosed ADHD.
Can treating ADHD reduce addiction risk?
Yes. Evidence from clinical trials shows that appropriate ADHD treatment, especially stimulant medication when started in childhood or early adulthood, is associated with lower rates of subsequent substance use disorder. Treating the root cause reduces the drive to self-medicate.
What is dual diagnosis?
Dual diagnosis refers to the co-occurrence of a mental health disorder and a substance use disorder in the same individual. ADHD and addiction are a common dual diagnosis pairing. Effective treatment addresses both conditions at the same time, rather than treating them separately or sequentially.
How do I know if I have ADHD alongside an addiction?
If you have struggled with addictive behaviours alongside lifelong difficulties with focus, impulsivity, emotional regulation, or organisation, there may be an underlying ADHD component. A formal ADHD assessment is the only way to know for certain.
ADHD and Addiction: Conclusion
The link between ADHD and addiction is real, well-documented, and deeply rooted in how the ADHD brain is wired. But it is not inevitable, and it is not permanent. Understanding that a neurological disorder—not weakness, laziness, or poor character—underlies much of the struggle can be both validating and transformative.
Whether you are managing an addiction and wondering if ADHD is part of the picture, or supporting someone whose ADHD seems to be driving compulsive behaviour, getting the right diagnosis is the most important step. It opens the door to treatment plans that actually address the root cause, not just the symptoms.
If this article has resonated with you, take our free ADHD self-test today, or reach out to our team to discuss whether a full assessment might be right for you.
References
1. Wilens, T. E. (2004). Attention-deficit/hyperactivity disorder and the substance use disorders: the nature of the relationship, subtypes at risk, and treatment issues. Psychiatric Clinics of North America, 27(2), 283–301. https://doi.org/10.1016/S0193-953X(03)00113-8
2. Lee, S. S., Humphreys, K. L., Flory, K., Liu, R., & Glass, K. (2011). Prospective association of childhood attention-deficit/hyperactivity disorder (ADHD) and substance use and abuse/dependence: a meta-analytic review. Clinical Psychology Review, 31(3), 328–341. https://doi.org/10.1016/j.cpr.2011.01.006
3. Koob, G. F., & Volkow, N. D. (2016). Neurobiology of addiction: a neurocircuitry analysis. The Lancet Psychiatry, 3(8), 760–773. https://doi.org/10.1016/S2215-0366(16)00104-8
4. Molina, B. S. G., & Pelham, W. E. (2003). Childhood predictors of adolescent substance use in a longitudinal study of children with ADHD. Journal of Abnormal Psychology, 112(3), 497–507. https://doi.org/10.1037/0021-843x.112.3.497
5. Charach, A., Yeung, E., Climans, T., & Lillie, E. (2011). Childhood attention-deficit/hyperactivity disorder and future substance use disorders: comparative meta-analyses. Journal of the American Academy of Child and Adolescent Psychiatry, 50(1), 9–21. https://doi.org/10.1016/j.jaac.2010.09.019
You Might Also Like
Contact Us
We’re here to answer any questions you might have.
Get in Touch
Opening Hours
Contact Form
We’re here to help. Reach out and we’ll get back to you within 24 hours (Monday – Friday).




Leave a Reply